When Medical Mission Sisters founder Anna Dengel arrived in Attat in the early 1960s to inspect an abandoned monastery where the Catholic church had asked her to consider starting a hospital, she immediately knew the answer: absolutely not.
Dengel took one look at the desolate rolling hills of south central Ethiopia and knew she could not send young sisters to a place where they would be so isolated. "She said, 'I can't send my sisters to where there is no road, no electricity, no nothing!'" recalled Sr. Inge Jansen, originally from Germany, who has lived in Attat for 47 years.
On the way out of Attat, Dengel and her party came across villagers who were carrying a woman in the throes of obstructed labor. They had been walking with the woman for three days in desperate search of medical help. The next place with a doctor was Addis Ababa, more than 100 miles (175 km) away, which would take days to reach. Dengel felt helpless. There was no way the woman could survive.
No one knows what happened to that nameless woman, though it is unlikely that she lived. But her presence changed the course of history for the Medical Mission Sisters in Ethiopia. Sisters from this community made their way to Attat from Germany and India, later the Philippines, America, Canada and Ethiopia. Starting from a mobile clinic carried on the backs of four rented mules, their facility and staff eventually grew to serve 70,000 patients per year. The operating theatre is state-of-the-art, located at the converted monastery classrooms.
Throughout the almost five decades of service, the main focus of the hospital has always been on maternal health: ensuring that every woman has the right and the ability to deliver healthy babies safely.
Ethiopia is the worldwide leader in addressing obstetric fistula, a medical condition when obstructed labor causes tears between the vagina and the rectum or bladder. The fistula is often the result of labor that has lasted for three days or more and leaves women incontinent in urine or feces or both. This incontinence is a source of overwhelming shame, and often leads a woman to be shunned by the community, levying a double blow against women who have often just lost a child.
The Hamlin Fistula Hospital in Addis Ababa trains doctors from developing countries around the world to perform the complicated operation to repair torn organs. The surgery can fix the fistula so that the women are no longer incontinent, and usually they can even go on to have more children. Attat, like many rural villages in Ethiopia and across Africa, had high incidences of fistula.
In northern Ethiopia, fistula can happen because girls are forced to get married at a young age, bearing children before their bodies have matured. In the Attat area in central and southern Ethiopia, early marriage is less common, but fistula was widespread due to labor complications. When women give birth in rural areas with few roads and scarce transportation, any problem during delivery means they are stuck. Previously, a woman in labor had to be carried to the nearest clinic on a makeshift stretcher. The longer she was in labor, the higher the probability of infant mortality and fistula.
"Fistula is an infrastructure problem," explained Sr. Rita Schiffer the lead OB-GYN of the hospital who has been in Attat for 19 years and was trained in fistula operations in Addis Ababa. Because fistula is the result of logistical challenges in the region and not cultural practices, it also means that the problem can be solved, with more roads, more transportation and a room filled with beds.
A logistical solution
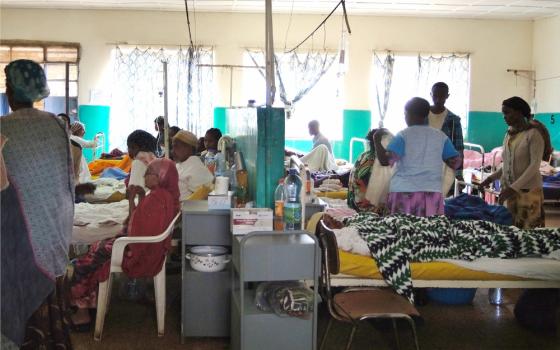
One of the first things the sisters did upon arriving in Attat was to open a "tulkum," a traditional round house with a thatched roof, on the hospital property. They filled the tulkum with beds and encouraged women in advanced stages of pregnancy to come stay there free of charge until they gave birth. The tulkum was especially important as prenatal care abilities increased at the hospital, and nurses could offer it as an option to women who showed signs of complicated deliveries.
"We started this from the beginning because, in a country with such poor infrastructure, you must have the high-risk mothers on your compound so they don't have a journey and don't have to look for transport. That is the solution," Schiffer said. "Instead of journeying a day or a day and a half, it's two minutes to the delivery room, and we're always ready for a C-section 24/7. After five minutes, if you need a C-section, you're on the table."
"Women themselves saw other women coming home rather than dying," said Sr. Elise Kurisummoottil, who has been at the Attat hospital for more than 25 years in two separate stints in the 1980s and 2000s.
The cost of the maternal waiting area is minimal, as women are expected to bring their own food to cook in a communal kitchen. Destitute women or those without families are given a meal ticket for the hospital canteen. Although their stay is free, it can be difficult for women to organize weeks of time away from their families.
In 2014, maternal mortality at Attat Hospital was 194 per 100,000 deliveries, while the overall maternal mortality rate in Ethiopia was 672. When Schiffer first arrived in the 1990s, she dealt with five to six cases of fistula each year, already a dramatic decrease from the amount prior to the maternal waiting area. Now, she sees one fistula case every two years.
Attat's success is being recognized on a national and international level. UNICEF has visited the hospital, to try to replicate the maternal waiting area and prenatal services in Ethiopia's impoverished Afar region, home to nomadic tribes. The government has taken notice of the hospital, replicating its public health outreach programs. "[The government] now encourages all women to come give birth in a hospital," Schiffer said. "[The campaign] is called 'Skilled Hands,' because everyone should deliver with the help of a midwife, at the minimum."
For the most part, women have readily embraced the government campaign, which has been very successful and led to a drastic decrease in maternal mortality. However, it has also led to a drastic increase in the amount of work for medical professionals.
In 2014, the hospital in Attat delivered approximately 1,800 babies. In 2015, after the Skilled Hands campaign was in full swing, this number increased to about 3,500. During one especially exciting 24-hour period in 2015, the six-doctor staff delivered 30 healthy babies.
The maternal waiting areas also offer an opportunity for health outreach. Public health workers give talks to expectant mothers on nutrition, immunizations, family planning, environmental hygiene, communicable diseases, malaria and harmful traditional practices such as female genital mutilation.
Schiffer and the other sisters cite two main reasons for their success in reducing fistula and maternal mortality. First is a combination of curative medicine coupled with teaching people hygienic and healthy practices at home. Second is a stable leadership that works slowly and patiently toward a common goal.
"If you're only doing curative, curative, curative health, nothing will change," said Sr. Antonia Redito, a doctor originally from the Philippines who has been in Attat for 33 years and now serves as the hospital operations manager. "It has to go hand in hand. The services we give here are integrated health and development services, because you have to do development work in the communities. The entry point is health, but everywhere you go, when you ask what they need, it's really water. Once you have safe water, then you're alive."
Clean water and stability
No matter how advanced the clinic became, the sisters knew they could not increase the level of basic health without improving the access to clean water. The Attat hospital has built 133 water projects in the hospital catchment area, including drilling boreholes, springs protection and hand-dug wells.
The water projects coupled with public health outreach about proper hygienic practices have significantly reduced the incidence of diarrhea and trachoma, a disease carried by flies that affects peoples' eyes. Trachoma causes the eyelashes to turn inward, scratching the cornea, which can cause blindness if left untreated. Fewer flies mean less trachoma.
When the sisters first opened the hospital, they were doing thousands of trachoma operations each year.
"The sisters were even doing these operations after supper so we could get enough done," Redito said. In the 1980s, this meant 3,000 to 4,000 trachoma operations per year.
With the water programs, when people have access to clean water to wash their faces, and better hygienic practices for toilet use, the incidence of trachoma plummeted. In 2014, the hospital did 198 trachoma operations.
Sisters also credit the stability of their leadership with the successful health operations. Among the international sisters, Schiffer is the newest, with 19 years at the hospital. Jansen has been in Attat for 47 years.
"When a group works in the same project it can really change things," Schiffer said, "instead of every 10 years, going in this direction and then in that direction. The continuity of a religious group is good for a project. Although the people may change, the direction or the priorities remain the same."
Sr. Belaynesh Abera is the first Ethiopian hospital director, though the hospital always had an Ethiopian assistant director. "The changes that this organization wants to bring about, they can do so because we are stable," she said. And after almost 50 years, the sisters see the results every day.
Improving basic health means the hospital is now dealing with what the sisters call "old people diseases" — diabetes, hypertension, stroke, heart disease, obesity. The focus, however, remains on helping women deliver healthy, happy babies.
"Women are coming into my office every day, saying, my baby was saved by being here," Abera said. At dinner, the sisters often discuss cases that tug at their heartstrings, happy stories as well as sad ones. "That is why our mission is here, that is why I'm here to contribute," she said. "I know what our contribution is, and it is so important."
Back in the maternal waiting room, a 35-year-old woman, who asked not to be identified, is waiting to give birth to her first child. It is her second pregnancy. Last time, she delivered in her village of Walga, an hour and a half from Attat. The birth was difficult, and the baby was stillborn. When she went for prenatal care at her local clinic this time, they referred her to Schiffer, who recommended that she stay at the maternal waiting area.
"I was not ready to stay," the woman said. "But for the sake of my life, and for the sake of my child, I am happy to be here."
[Melanie Lidman is Middle East and Africa correspondent for Global Sisters Report based in Israel.]
Related - Q & A with Sr. Dr. Antonia Redito, ministering in Ethiopia no matter the method