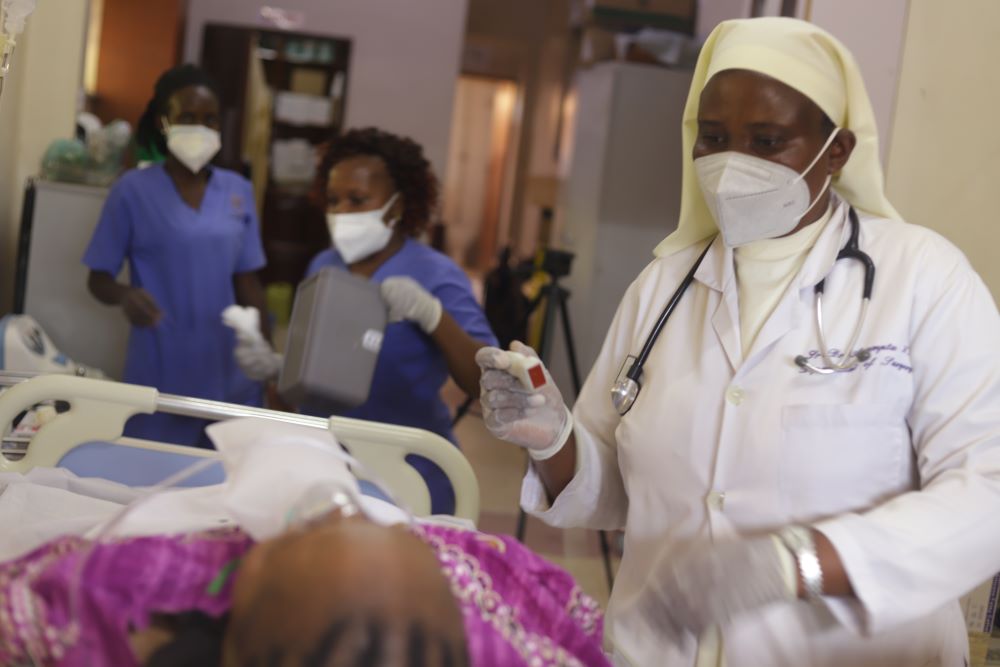
Sr. Assumpta Nabawanuka attends to a patient at St. Francis Hospital Nsambya in Kampala, Uganda's capital. Nabawanuka, a member of the Sisters of the Immaculate Heart of Mary Reparatrix – Ggogonya, said she used her long medical experience to lead a team of health care workers during COVID-19. (GSR photo/Doreen Ajiambo)
Sr. Assumpta Nabawanuka, a medical doctor at St. Francis Hospital Nsambya in Kampala, Uganda, used her long medical experience to lead a group of health care workers at the facility to tackle COVID-19 when the first case was confirmed March 21, 2020.
Nabawanuka, whom many residents here say is a hero of the pandemic, is a member of the Sisters of the Immaculate Heart of Mary Reparatrix – Ggogonya. She was among the team selected and trained by the government of Uganda through the Ministry of Health to deal with COVID-19 patients who were flooding hospitals at the time.
Nabawanuka worked in several other hospitals before she ended up at St. Francis Hospital Nsambya, a referral hospital with 361 beds. According to its website, the hospital, which is involved in patient care, research and teaching, "offers specialist services in surgery, internal medicine, pediatrics, obstetrics and gynecology."

St. Francis Hospital Nsambya, commonly known as Nsambya Hospital, is a Catholic mission hospital owned by the Archdiocese of Kampala and managed by the Little Sisters of St. Francis of Assisi. (GSR photo/Doreen Ajiambo)
Founded in 1903, the hospital has general and private patient facilities and is owned by the Archdiocese of Kampala and run by the Little Sisters of St. Francis of Assisi. Nabawanuka is the head of the facility's trauma and emergency department.
The East African country of over 45 million people has more than 165,000 confirmed cases of COVID-19 and 3,613 confirmed deaths. The most recent health records from the Ministry of Health show that 39% of people have received at least one vaccine dose, and 31% are fully vaccinated.
GSR: How did you find yourself at the forefront of the fight against COVID-19 in Uganda?
Nabawanuka: I was among the team that the government selected to deal with COVID-19 cases. We got COVID-19 at a point we were not expecting it, and of course, we didn't know which kind of disease it was at the time. The Ministry of Health selected a few people from different hospitals to train them about the disease. I was among those who were chosen to be trained about the disease and management of the disease. In fact, I was involved in drafting protocols for COVID-19 for the hospitals.
How was the COVID-19 situation in the country at the time, and how did you handle it?
At the beginning of the pandemic, we received an overwhelming number of people with COVID-19 infections. I can't give a specific figure on it, but it was overwhelming.
The intensive care unit beds at the public hospitals were fully occupied. In fact, we were not allowed by the government to treat COVID-19 patients at our private facility [at first]. We would take the patients to government hospitals. But with the overwhelming numbers, we were allowed to treat the patients.
The situation was challenging and emotional. As a doctor, I managed the patients directly in screening and treatment. At the peak of the pandemic [around June to December 2020], we were losing a significant number of patients. I had to call a priest to bring anointing for the patients and pray for them so that God could do something. I think most of the patients who finally died because of COVID-19 died peacefully because we used to give them hope through the word of God.

Sr. Assumpta Nabawanuka, center, and two nurses visit patients admitted at St. Francis Hospital Nsambya in Kampala, Uganda's capital. Nabawanuka, a member of the Sisters of the Immaculate Heart of Mary Reparatrix – Ggogonya, was among the team selected by the government of Uganda to deal with COVID-19 when the first case was confirmed on March 21, 2020. (GSR photo/Doreen Ajiambo)
What are some of the emotional moments you experienced while working with COVID-19 patients?
Right now, we have an insufficient number of COVID-19 patients. They are still there, but [we are down to] remnants.
When the pandemic was at its peak, many patients died as we watched helplessly. COVID-19 was new to us, but we tried to study it in a very short time. Being the head of the department, I had to be strong and lead a team of health care workers to battle the disease. If I left or became demoralized in handling the disease, others would have run away from the patients, which would have been catastrophic.
I remember when the first COVID-19 patient we received at the facility died. The patient had visited the facility before, but none of us knew at the time that he was COVID-19 positive. When we did the PCR test on his body, we discovered he was a positive case. Everyone who had touched the patient was scared, but I had to remain strong because I was leading the team. So I had to stand in, find the solution to that problem and keep the team strong.
After that experience, we treated patients, and I tell you, the situation was terrible. I was with the team here at the hospital, engaging them, discussing, training and treating them.
What are some of the challenges you went through at the peak of the pandemic?
We had a lot of pressure on us. We had to treat the patients and handle the emotional part of the health workers and some of our staff. We had to do a lot of counseling and engagements with the team for them to deal with the disease. They were demoralized, scared and almost giving up. But as a health practitioner, much was expected. We gave out more than what we got. But we thank God. He led us through those challenges.
Advertisement
How did you deal with vaccine hesitancy among health workers and patients visiting the facility?
When the vaccines came, we had to be at the forefront. Some of the nurses and doctors at our facility didn't believe in the vaccines. I had to take it upon myself to convince them to accept the vaccines and get vaccinated. I told them they could not go out there and tell citizens to receive vaccines if they don't trust the vaccines themselves. The medical practitioners had to accept the vaccines first and learn how to handle and administer them before we could vaccinate other people.
I ensured that people knew about the vaccines and how they would benefit them. But people had a lot of fear about the vaccines. They had a lot of myths surrounding the vaccines that made them fear more. But I began to talk to them wherever they would visit the facility, and sometimes, I would go and speak to the community.
Shockingly, they started accepting them with time. Many told me they accepted being vaccinated because I was a religious sister, and they believed in us. Some people wanted to be treated or vaccinated by the sisters only, which increased our work.
Anything else you would like to share with us?
We have achieved a lot because many people have been vaccinated, and vaccination is still going on. As religious sisters, we have done a lot to ensure people are vaccinated. We talk to them and encourage them to get vaccinated.
The fight against the pandemic has been quite an experience for me. We are busy in the laboratories trying to develop another vaccine made by us, medical practitioners, to support the government.
As a religious sister, I believe in God. The Holy Spirit is active and has worked with us throughout the pandemic period. Treating a new disease and doing what we did was because of God. We would have run away from this pandemic, but the Holy Spirit kept us strong.







